Platelet-rich plasma (PRP)
EVALUATION
EVALUATION
What is PRP? How does it work, and when can it be used?
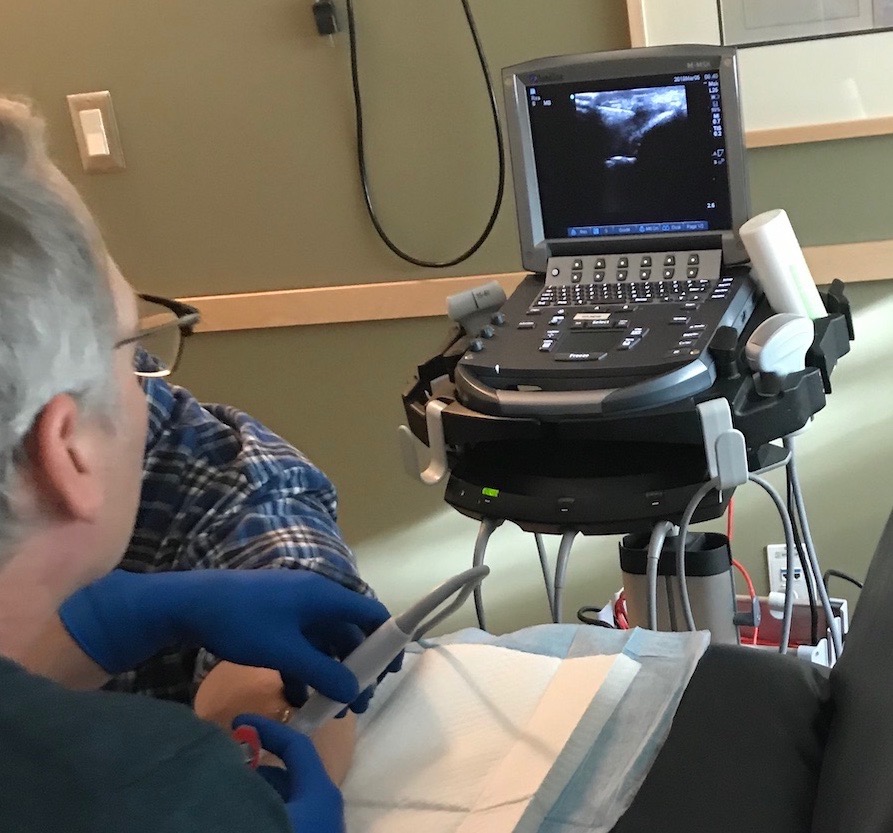
WHAT. Platelet-rich plasma (PRP) is derived from a blood sample collected from the patient (autologous). The patient’s blood is first drawn and centrifuged. The red blood cells are then discarded yielding a high concentration of platelets, in the remaining plasma which release numerous growth factors and proteins. The PRP is then injected into the patient at the site of injury in order to promote healing. Ultrasound guidance is often used to increase the accuracy of the injection.
HOW. Growth factors and proteins released from platelets influence healing by stimulating blood flow to tissues, removing damaged cells at the injury site, and promoting the growth of normal tissue. It has been shown to have positive effects on cell growth and proliferation of stem cells by increasing anti-inflammatory mediators and decreasing proinflammatory mediators. PRP treatment has shown to influence the healing of tendon, ligament, muscle, and bone.
WHEN. PRP may be used in both acute injuries (less than 90 days old) and chronic injuries
(greater than 90 days old) to accelerate the healing of tissues. PRP can be useful in osteoarthritis, Achilles and patella tendinopathy, hamstring injuries, rotator cuff disease, epicondylitis, and degenerative spine disease. PRP may be considered by the patient for the treatment of these various musculoskeletal injuries in conjunction with other therapies (e.g. physical rehabilitation, acupuncture, chiropractic) or as another option when those therapies have failed. Patients should avoid the use of nonsteroidal anti-inflammatory drugs ten days prior and ten days after the administration of the injection in order to maximize the efficacy of the injection.
*When considering PRP it is important to note that clinical studies have yielded both beneficial effects of PRP as well as inconclusive results. More controlled clinical trials are warranted for a better understanding of the full capacity of PRP treatment.
